Self-stimulatory behavior, also known as stimming and self-stimulation, is the repetition of physical movements, sounds, or words, or the repetitive movement of objects
Stimming – Wikipedia
Autistic adults highlighted the importance of stimming as an adaptive mechanism that helps them to soothe or communicate intense emotions or thoughts and thus objected to treatment that aims to eliminate the behaviour.
‘People should be allowed to do what they like’: Autistic adults’ views and experiences of stimming – Steven K Kapp, Robyn Steward, Laura Crane, Daisy Elliott, Chris Elphick, Elizabeth Pellicano, Ginny Russell, 2019
We have five external senses:
- Taste
- Smell
- Touch
- Sight
- Hearing

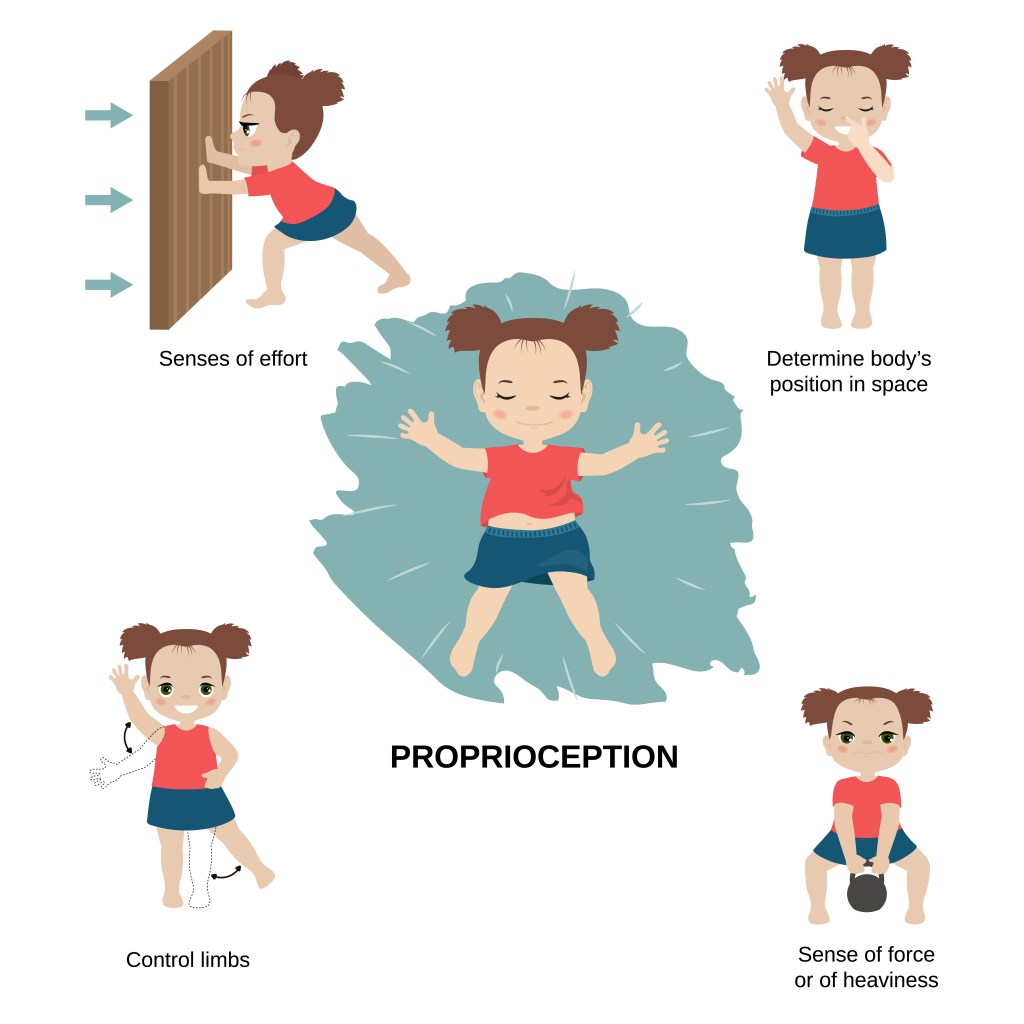
And three internal senses:
- Proprioception
- Vestibular
- Interoception
We engage those senses with stimming for a few reasons:
- Self-regulation
- Sensory seeking
- Expression

Autistic sensory differences
| Sensation | Considerations |
|---|---|
| Sight | Visual sensitivities are common. Bright lighting (particularly fluorescent) is a common challenge. Visual stimuli which may go unnoticed by non-autistic people, such as the flickering of fluorescent lighting or computer screens, an overhead rotary fan, or highly patterned surfaces, may all cause sensory stress |
| Sound | Autistic people experience auditory sensitivities and auditory processing differences. Environmental noise can cause intense distress, particularly when sudden or unexpected. Sounds unnoticed by non-autistic people, such as the humming of electrical equipment, may be perceived by autistic people without ‘fade’ (where inconsequential sounds are no longer noticed over time). Autistic people may not filter out environmental sounds and therefore may struggle to hear a conversation in a noisy room |
| Smell | Autistic people are often highly sensitive to smell and may perceive olfactory stimuli that others do not. Common and usually inoffensive smells may be perceived as highly noxious. In contrast, some autistic people are hyposensitive to smell and may enjoy smelling pungent objects |
| Taste | Autistic people may be hypo- or hyper-sensitive to taste, needing either highly flavoured or very bland food. Food texture is important, as is predictability (see below). Autistic people commonly enjoy colloquially termed ‘same foods’, which may explain a limited diet and negative reactions to a change of brand or recipe for a known brand of food |
| Touch | Tactile sensitivities range from inability to tolerate the sensation of certain fabrics to an inability to be touched, particularly by strangers. This leads to predictable challenges in a medical consultation where physical examination is required. Knowing the tactile sensitivity profile of a patient is helpful because difficulties commonly arise with light touch, whereas a strong deep touch may be more acceptable |
| Temperature | Thermal sensitivity is common and may lead to apparently inappropriate or out of season clothing. The range of tolerated temperatures is likely to be person-specific |
| Proprioception | Proprioception appears different for autistic people. Some may need lots of proprioceptive input leading to a tendency to climb, swing, rock or jump. Others will avoid such movements and may experience balance difficulties during day-to-day activities |
| Interoception and pain | A particular challenge for some autistic people is accurately interpreting internal bodily sensations. This can lead to difficulties noticing hunger, thirst, tiredness, or a need to urinate or defaecate. Difficulties with pain perception can lead to unrecognised injuries but it must be emphasised that while reduced pain sensitivity occurs for some, others experience increased pain sensitivity, and this should never result in under-treatment of pain for autistic patients |
Recommendations for supporting Autistic sensory needs
Autistic SPACE: a novel framework for meeting the needs of autistic people in healthcare settings | British Journal of Hospital Medicine
- Sensory needs.
- Predictability.
- Acceptance.
- Communication.
- Empathy.
| SPACE framework aspect | Recommendations for implementation | |
|---|---|---|
| Sensory | Sight | Turn off or turn down artificial lights |
| Remove flickering or oscillating environmental features | ||
| Avoid highly stimulating decor | ||
| Promote the use of sunglasses | ||
| Sound | Consider environmental sounds | |
| Reduce auditory clutter | ||
| Avoid conversation in noisy environment | ||
| Promote the use of noise-cancelling headphones and/or ear plugs | ||
| Smell | Avoid wearing perfume or highly scented cosmetics or toiletries | |
| Avoid aerosols or chemical ‘air fresheners’ | ||
| Avoid highly scented cleaning products | ||
| Consider ventilation, open windows where possible | ||
| Taste | Respect sensory preferences when considering nutrition | |
| Consider taste and texture of medications | ||
| Consider non-standard medication formulations where necessary | ||
| Touch | Ascertain tactile preferences and modify examination technique | |
| Avoid casual touch | ||
| Promote sensory-friendly clothing choices | ||
| Sensory aids such as weighted blankets may be helpful | ||
| Temperature | Consider environmental temperature | |
| Adjust temperature where required | ||
| Proprioception | Understand the need for proprioceptive input | |
| Avoid making inferences from unusual body posture | ||
| Interoception and pain | Ask directly about internal sensations but understand that answering may be difficult | |
| Pay attention to verbal reports of pain where possible | ||
| Be aware that non-verbal expression of pain may be different | ||
| Consider the need for adapted pain scales | ||
| Predictability | Give realistic information in advance | |
| Ensure clear and accurate directional signage in physical spaces | ||
| Provide photographs or videos of the physical environment and staff | ||
| Allow waiting in a familiar environment (eg a patient’s own car or outside) | ||
| Ensure care is provided by staff familiar to the patient where possible | ||
| Acceptance | Neurodiversity-affirmative approach beneficial | |
| Understand autistic stimming and monotropic thinking patterns | ||
| Facilitate need for detailed factual information | ||
| Understand distress behaviour | ||
| Communication | Understand autistic verbal and non-verbal communication differences | |
| Know that communication ability is reduced by anxiety and sensory stress | ||
| Clear unambiguous communication required | ||
| Avoid phone-based appointment systems | ||
| Promote use of augmentative and alternative communication (AAC) | ||
| Empathy | Recognise that autistic people feel empathy but may display it differently | |
| Empathy towards autistic patients may be more challenging for non-autistic healthcare providers | ||
| Physical space | Expect a need for increased personal space | |
| Avoid proximity to other people where possible | ||
| Temporal space | Allow increased time to respond to questions | |
| Allow increased time for decision making | ||
| Emotional space | Expect differences in emotional expression | |
| Allow restorative solitude to recover (without additional input) if distressed | ||

while stimming I am able to unravel the everyday ordinary barrage of sensory and social information that becomes overwhelming.
The Predictability, Pattern and Routine of Stimming | Judy Endow
Most of us stim because it calms us and helps alleviate our high levels of anxiety.
Siena Castellon
We have five external senses and three internal senses. All must be processed at the same time and therefore add to the ‘sensory load’.
Understanding the sensing and perceptual world of autistic people is central to understanding autism.
Autism is viewed as a sensory processing difference. Information from all of the senses can become overwhelming and can take more time to process. This can cause meltdown or shutdown.
“It’s Not Rocket Science” – NDTi
The film was commissioned by Manchester Collective in response to Michael Gordon’s ‘Weather’ as part of “Northern Voices”. The film was shown as part of a live performance of ‘Weather’ at the RNCM.
Interview with Nia Thomas about the piece: https://manchestercollective.co.uk/sophie-broadgate-in-motion
The interconnectedness between sensory input, emotions, energy level, ongoing task and how you manage everything you have to do alongside coping with sometimes overwhelming sensory input is an experience that many autistic people are familiar with. Understanding just how much the sensory world can impact how anxious you feel, how well you can communicate, how able to do a food shop or even just enter a space is an important piece of understanding to build up. Without this understanding, from the perspective of autistic people, many may not understand how all-consuming the sensory environment can be for some and for others it is a way of being able to interact that releases anxiety and tension. Interacting with the sensory world through sensory seeking behaviours is strongly associated with stimming (self-stimulatory behaviour that helps self-regulation) which is often a really positive (as long as no one is getting hurt) way of expression that can encompass happiness, anxiety, distress and so much more.
Autistic sensory experiences, in our own words — Sarah O’Brien
We’re Autistic. Here’s what we’d like you to know.
I will never understand how people can justify the use of “quiet hands”. If you are unaware of what this phrase means, or of the implications for autistic people, you need to read Quiet Hands by Julia Bascom.
When a parent, sibling, educator, therapist, medical professional, etc justifies the use of quiet hands, it baffles me. Do they understand what stimming is? Do they realize that my hands are the key to helping me see the world? Or do they just see my movements as separate from me, as a source of embarrassment for them? I tend to think it’s the latter, that it’s because stimming draws unwanted attention that people want to quiet my hands in the first place. They don’t understand the point of stimming, or I think (hope) they wouldn’t try and prevent it.
So this is what happens when you “quiet hands” us. It’s the equivalent to duct taping an NT person’s mouth shut or preventing a nonspeaking D/deaf person from signing. You are taking away our natural language. You make interacting with the world that much harder.
On Stimming and why “quiet hands”ing an Autistic person is wrong
Autistic adults highlighted the importance of stimming as an adaptive mechanism that helps them to soothe or communicate intense emotions or thoughts and thus objected to treatment that aims to eliminate the behaviour.
Furthermore, more recent theories have suggested that stimming may provide familiar and reliable self-generated feedback in response to difficulties with unpredictable, overwhelming and novel circumstances (e.g. Lawson, Rees, & Friston, 2014; Pellicano & Burr, 2012). As such, stimming may provide not only relief from excessive sensory stimulation, but also emotional excitation such as anxiety (Leekam, Prior, & Uljarevic, 2011). Consistent with these suggestions, autistic adults report that stimming provides a soothing rhythm that helps them cope with distorted or overstimulating perception and resultant distress (Davidson, 2010) and can help manage uncertainty and anxiety (e.g. Joyce, Honey, Leekam, Barrett, & Rodgers, 2017).
Autistic people have become increasingly mobilised and vocal in defence of stimming. Autism rights or neurodiversity activists believe that stims may serve as coping mechanisms, thus opposing attempts to eliminate non-injurious forms of stimming (e.g. Orsini & Smith, 2010). They decry practices such as ‘quiet hands’ (which teaches the suppression of hand flapping), instead using ‘loud hands’ as a metaphor both for using such non-verbal behaviour to communicate and for cultural resistance more broadly (Bascom, 2012). In addition, autistic scholar-activists denounce attempts to reduce their bodily autonomy (Nolan & McBride, 2015; Richter, 2017) and declarations of their stimming as unacceptable or as necessarily involuntary (Yergeau, 2016).
‘People should be allowed to do what they like’: Autistic adults’ views and experiences of stimming – Steven K Kapp, Robyn Steward, Laura Crane, Daisy Elliott, Chris Elphick, Elizabeth Pellicano, Ginny Russell, 2019
My son stims. He performs repetitive motions in order to generate sensory inputs that he experiences as fun, aesthetically pleasing, soothing, exciting, or otherwise necessary. The word comes from the clinical term, “self-stimulatory behavior,” but there’s no need to be that clinical about it. His stimming is beautiful. To get him to stop stimming would require intensive coercion that, even if successful, would likely result in irreparable psychological harm.
What Applied Behavioral Analysis Gets Wrong About Stimming and Children – Pacific Standard
Calming, Soothing, Focusing, Joy-Inducing
“Stimming is a way that we can help ourselves feel calm, soothed, or focused, but it can also be a huge source of joy and beauty.”
What Applied Behavioral Analysis Gets Wrong About Stimming and Children – Pacific Standard
The first part is in my “native language,” and then the second part provides a translation, or at least an explanation.
But my language is not about designing words or even visual symbols for people to interpret. It is about being in a constant conversation with every aspect of my environment. Reacting physically to all parts of my surroundings.
In My Language
Many people with autism are stressed individuals who find the world a confusing place (Vermeulen, 2013). So how does someone with autism achieve a sense of flow? McDonnell & Milton (2014) have argued that many repetitive activities may achieve a flow state. One obvious area where flow can be achieved is when engaging in special interests. Special interests allow people to become absorbed in an area that gives them specialist knowledge and a sense of achievement. In addition, certain repetitive tasks can help people achieve a flow like state of mind. These tasks can become absorbing and are an important part of people’s lives. The next time you see an individual with autism engaging in a repetitive task (like stacking Lego or playing a computer game), remember that these are not in themselves negative activities, they may well be reducing stress.
If you want to improve your supports to people with autism from a stress perspective, a useful tool is to identify flow states for that person and try to develop a flow plan. Remember, the next time you see a person repeating seemingly meaningless behaviours, do not assume that this is always unpleasant for them – it might be a flow state, and beneficial for reducing stress.
What is ‘flow’?

